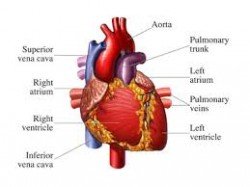
 The heart is constructed of four chambers: the right atrium and the right ventricle, and the left atrium and the left ventricle. These four chambers function as two side-by-side pumps, each of which sends blood through a completely different system of circulation. The right side of the heart pumps blood through the less forceful pulmonary circulation of the lungs, where oxygen-depleted blood is replenished in lung tissue with oxygen from the air we breathe.
The heart is constructed of four chambers: the right atrium and the right ventricle, and the left atrium and the left ventricle. These four chambers function as two side-by-side pumps, each of which sends blood through a completely different system of circulation. The right side of the heart pumps blood through the less forceful pulmonary circulation of the lungs, where oxygen-depleted blood is replenished in lung tissue with oxygen from the air we breathe.
The left side of the heart pumps blood into the rest of your blood vessels, allowing nourishing, oxygen-rich blood to leave the heart and travel throughout the rest of the body. The atria receive blood from the body on the right side and from the lungs on the left side. The two ventricles are the pumping chambers that expel the blood. The two pumps operate in synchronized fashion, the two atria and then the two ventricles contracting and relaxing simultaneously.
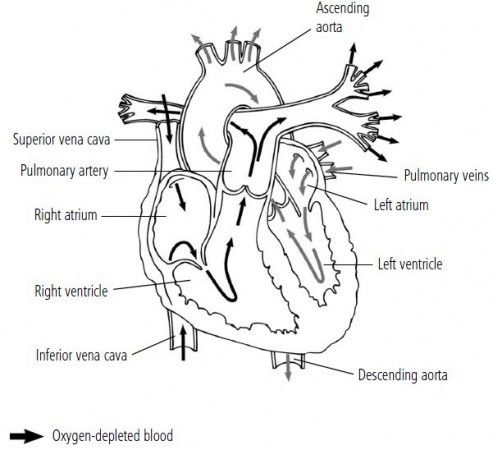
The four chambers of your heart function as two side-by-side pumps. On the right side, oxygen-depleted blood that has circulated through the body passes into the right atrium through the superior vena cava and inferior vena cava. The right atrium pushes it into the right ventricle, which moves it into the pulmonary artery to flow into the lungs. In the lungs, the blood is enriched with fresh oxygen. Then the oxygen-rich blood flows through the pulmonary vein into the left side of the heart. The left atrium sends the blood into the left ventricle, which contracts forcefully enough to pump the blood into the aorta, the major artery at the top of the heart. From the aorta, the oxygen-rich blood is distributed throughout the body to nourish cells.
The two sides of the heart are separated by a thick muscular wall called the septum, which prevents blood from passing directly from one side of the heart to the other. To understand the mechanics of pulmonary (lung) circulation, you can trace the path of about half a cup of blood —the amount pumped in a given heartbeat— through the right side of the heart.
Blood enters the right atrium of the heart through two large veins: the superior vena cava, which collects blood from your head and upper body, and the inferior vena cava, which collects blood from your legs and abdomen. At this point, the red blood cells in the blood returningto the right atrium have delivered oxygen and nutrients to other body tissues. The depleted blood has a low oxygen content. The right atrium contracts and sends the blood through a one-way valve into the right ventricle, which in turn contracts and pushes the blood out through the pulmonary artery into the lungs. As the blood circulates through the lungs, it unloads carbon dioxide, a waste product of cellular function that it has carried from body tissues. The red blood cells then pick up fresh oxygen, and the blood is enriched, or oxygenated.
Similarly, on the upper left side of the heart, circulation to the rest of your body starts with the left atrium. Bright red, oxygen-rich blood enters the chamber via the pulmonary vein, from the lungs. The walls of the left atrium contract and push the
blood through a one-way valve into the left ventricle. Then the left atrium relaxes while the powerful left ventricle contracts with the considerable force required to propel the blood into the aorta—the major artery at the top of the heart that directs the blood throughout the body. The left ventricle is the main pump and the strongest muscle tissue in the heart.
The Heart Valves
The blood flow through the heart needs to be one-way and carefully regulated. Four one-way valves between the chambers ensure that the blood moves through the heart and lungs in sequence and never dams up or back-flows. All the heart valves are constructed of overlapping flaps (leaflets or cusps) that open and close to control blood flow.The valves differ by structure and function.
The pulmonary and aortic valves between a ventricle and the great artery are called the semilunar valves because of their crescent-shaped leaflets. The tricuspid and mitral valves between the right and left atria and a ventricle are also called atrioventricular valves. The leaflets of the two atrioventricular valves are attached to the ventricular walls by fibrous cords. When the ventricle contracts and the valve closes, the cords secure the leaflets in place so they are not blown backward by the force of the contraction.
The tricuspid valve, on the right side of the heart, is named for its three leaflets, or cusps. Returning, oxygen-depleted blood flows through this valve into the right ventricle. As the blood flows out of the right ventricle and into the pulmonary circulation, it passes through the pulmonary valve. The pulmonary valve’s three leaflets open as the right ventricle contracts and close again as it relaxes.
As the oxygen-enriched blood passes back into the left atrium, it passes through the mitral valve (named for its shape, which resembles a type of bishop’s hat called a miter). This valve has just two highly mobile cusps that can close rapidly when the powerful left ventricle contracts. This valve is attached by cords to muscles within the ventricle. Finally, as the blood flows out of the left ventricle and into the aorta, the three-part aortic valve opens against the walls of the aorta. When the blood has passed into the aorta, the valve falls shut.
The Heartbeat
The continuous function of your heart is probably easiest to understand if you break it down into a single unit of pumping action, the heartbeat. A healthy heart beats between 50 and 75 times per minute, so a single heartbeat may occur in less than a second. It involves two distinct phases, the systole and the diastole. The systole is the pumping phase and the diastole is the resting phase.
The systole actually occurs in two sequential pumping actions: the atrial systole and the ventricular systole. The lub-dub that is heard through a stethoscope is the sound of the heart valves closing during the heartbeat’s pumping cycle. The first heart sound, the “lub,” coincides with the closing of the mitral and tricuspid valves. The second heart sound, the “dub,” occurs with the closing of the aortic and pulmonary valves.
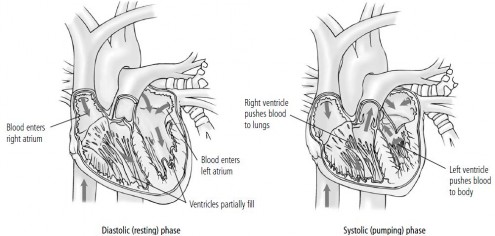
A single heartbeat moves a quantity of blood through the heart in two phases: a resting, or dilating (diastolic), phase and a pumping, or squeezing (systolic), phase. During the diastolic phase, the heart relaxes and fills, as oxygen-depleted blood flows into the right atrium from the body, and oxygen-rich blood flows from the lungs
into the left atrium. The ventricles fill partially. Then, during the systolic phase (right), an electrical impulse causes the heart to contract. First, the atria contract and completely fill the ventricles with blood. Then the ventricles contract, pumping blood out of the heart.
The diastole, the first and longer resting phase, occurs as blood collects in the two (right and left) atria. In the right atrium, depleted blood enters from the body, and in the left atrium, oxygen-rich blood flows in from the lungs. Systole begins when an electrical signal from the heart’s pacemaker cells stimulates the atria to contract and empty. The tricuspid and mitral
valves open and blood flows into the two ventricles.
When the ventricles are full, the electrical impulse passes into an area just above the ventricles and triggers the ventricular systole, the third and final step. All four valves are in action: the tricuspid and mitral valves close to prevent backflow from the ventricles to the atria, and the pulmonary and aortic valves are pushed open as blood surges out. On the right side of the heart, oxygen-poor blood travels from the right ventricle into the pulmonary artery on its way to the lungs to acquire oxygen. On the left side of the heart, oxygen-enriched blood flows from the left ventricle through the aorta and into the general and coronary circulation.
After the blood has left the ventricles, they relax, and the pulmonary and aortic valves close. As the ventricles relax, the pressure in the ventricles lowers, allowing the tricuspid and mitral valves to open, and thecycle begins again. Throughout this cycle, the two adjacent pumps move exactly the same amounts of blood; the volume of blood that enters and leaves the right chambers is the same as the volume that passes through the left chambers. Any change in the amount of blood entering the right side of
your heart—in response to exertion, stress, or temperature changes, for example—causes a corresponding change in the amount of blood passing through the left side. Your brain is constantly monitoring the conditions that might require a change in blood supply and adjusting your heart’s function accordingly.
The Heart’s Electrical Conduction System
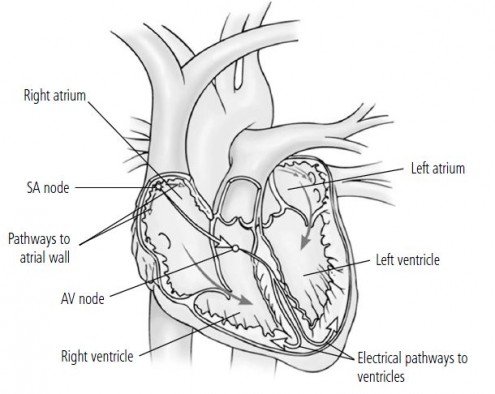
Your heart’s electrical activity Areas of specialized cells in heart tissue can initiate and conduct electrical impulses. The sinoatrial (SA) node, an area of electrical cells at the top of the right atrium, fires an impulse that initiates each heartbeat. The impulse first stimulates the walls of the atria to contract, allowing blood to fill the ventricles, and then travels to the atrioventricular (AV) node (over the ventricles). The AV node acts as a relay station for the signal beforepassing the impulse into the ventricles via branching electrical pathways.
The electrical activity that stimulates and paces the heartbeat is critical. In order to deliver an appropriate blood supply to body tissues, the heart must beat at an adequate rate, and the timing and sequence of muscular contractions must be precisely coordinated. Your heart’s natural pacemaker is the sinoatrial (SA) node, a microscopic group of specialized electrical cells located at the top of the right atrium. Each heartbeat originates in the SA node when it fires off an electrical impulse. This impulse travels via specialized pathways to the cells in the muscle tissues of the heart wall.
The impulse first stimulates the upper chambers, the atria, to contract and squeeze blood out into the ventricles. Then the impulse moves to another area of electrical cells called the atrioventricular (AV) node, located over the ventricles. This node acts as a relay station, allowing for a brief interval during which the atria empty completely before releasing the impulse along branching pathways that travel to the two ventricles to stimulate ventricular contraction.
The ventricles similarly contract and empty, and blood is pumped into the pulmonary artery and the aorta. The SA node speeds up when your body needs more blood. It also slows down during rest or in response to some medications. The message to increase or decrease the rate of impulses is controlled by the autonomic nervous system—the part of the nervous system that controls unconscious, automatic body functions including heart rate, blood pressure, and breathing. Autonomic nervous system activity regulates the release of the hormones epinephrine and norepinephrine, which act as accelerators for the heart’s electrical impulses during times of stress or exercise.
Your heart’s electrical activity can be followed and recorded on paper as an electrocardiogram. The initial impulse from the SA node is seen as a wave on the electrocardiogram, followed by a more static interval. The electrocardiogramrecording shows spikes as the impulse travels from the AV node through the ventricular pathways and is again followed by a static interval that is a segment of recovery.
Coronary Circulation
Because your heart must operate continuously to supply the rest of your body with blood, it works harder and requires a richer blood supply of its own than any other muscle in your body. It cannot extract oxygen and nutrients from the blood that moves through it, so it maintains its own dedicated circulatory system of arteries and veins. This coronary circulation begins with two coronary arteries that branch off of the aorta just above the aortic valve (on the left side). These arteries extend over the surface of the heart and branch into smaller vessels that penetrate the heart muscles to provide oxygen. After the muscles of the heart
have been nourished, the blood travels through coronary veins into the coronary sinus and then the right atrium. At this point, it flows in with the oxygen-depleted blood from the rest of the body.
The left coronary artery supplies blood to most of the powerful left ventricle. The circumflex coronary artery is really a branch of the left coronary artery. It wraps around the back of the heart and has several smaller branches. The right coronary artery supplies part of the left ventricle and most of the right ventricle. Interestingly, the configuration and even the sizes of the coronary arteries differ significantly from person to person.
The coronary arteries deliver oxygen-rich blood to the cardiac muscle cells according to the demand at the moment. If you are exerting yourself physically, your heart beats faster and more vigorously, and your coronary arteries expand to allow greater blood flow.
Your Heart’s Performance
Both the rate at which your heart beats and the volume of blood your heart moves in a single beat determine how efficiently your heart pumps blood. Cardiologists calculate cardiac output to measure your heart’s efficiency. Cardiac output is, quite simply, the amount of blood your heart pumps through your circulatory system in one minute. It is calculated by multiplying how much blood the left ventricle squeezes out in a single contraction (stroke volume) by the number of times the heart
contracts in a minute (heart rate).
Most typically, when your body needs more blood (for instance, when you are running up stairs) the heart increases its output by beating faster. If your heart beats at a fast rate for very long, the muscle begins to tire and the resting phase of the heartbeat becomes too short for the chambers to fill adequately. If you are physically fit, your heart muscle is stronger and can pump more blood with each contraction.
That is, your stroke volume is higher, so your heart can deliver adequate blood to your body without tiring as quickly. A physically fit person may actually have a low resting heart rate, because he or she has strengthened the heart muscle so that it can pump more blood, delivering adequate oxygen to the body with fewer strokes. When a fit person exercises, he or she may have the same heart rate as someone who is less fit, but the fit person is able to do more work, such as run longer without
tiring.
A healthy resting heart rate is usually between 50 and 75 beats per minute. When you exercise, your heart rate may increase to as much as 165 beats or more. Age plays a role in determining your maximum heart rate; the maximum number of beats per minute can be very roughly predicted by the formula 220 minus your age. A number of other factors can cause your heart rate to increase, including stress, some medications, caffeine, alcohol, and tobacco. When a healthy person sleeps, his
or her heart rate may dip to as low as 40 beats per minute. As you age, your heart rate may decrease somewhat.
Stroke volume in most people is about 3 ounces. That means that the ventricles pump out about half the blood they contain. A good athlete may be able to increase his or her stroke volume by 5 percent or more. A diminishing stroke volume is one of the first signs of a failing heart.
A pregnant woman’s body demands more blood flow and oxygen for the developing placenta. Stroke volume increases early in pregnancy, and later the heart rate increases to maintain a cardiac output 40 to 50 percent above normal. These changes reverse after the baby is delivered.